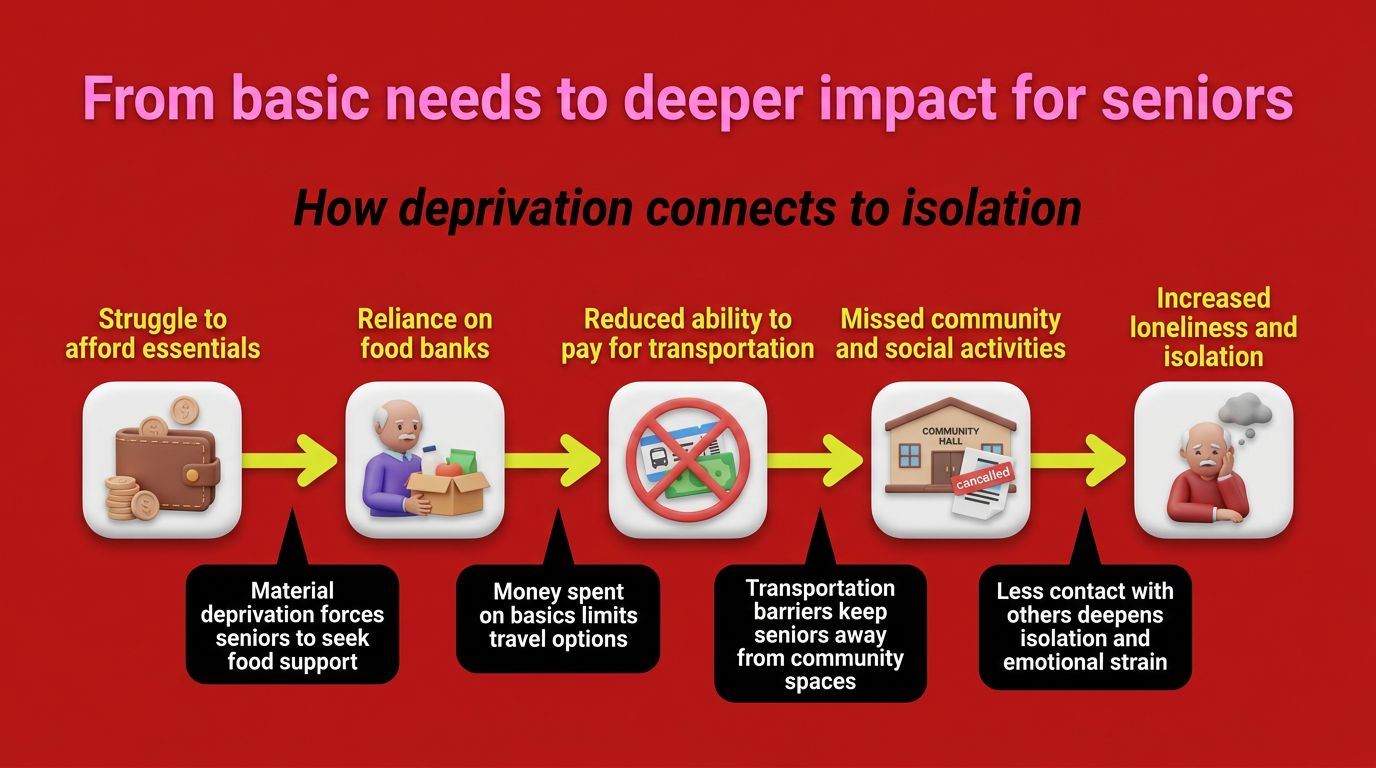
For older Ontarians, food insecurity is not abstract. It is the day the rent goes up and the fridge stays empty. It is the dental bill that wipes out the grocery budget. A recent national survey of more than 6,000 people aged 50 and over found that about 20 per cent are experiencing material deprivation, struggling to cover essentials like food, heat, dental care and small emergency costs.
That same work found that 18 per cent could not handle an unexpected 500 dollar expense and 11 per cent could not afford dental care. When basic needs are that fragile, food banks become part of the monthly routine for seniors, not a rare last resort. Use of food banks by older adults has already risen 35 per cent since 2023, a signal that the floor is giving way under too many elders.
Food insecurity is only half of the story. Forty-three per cent of Canadians over 50 are at risk of social isolation and 57 per cent report feeling lonely. When someone cannot afford a bus ticket across town, they do not just skip a community lunch, they lose the conversation, the laughter and the simple human contact that keeps depression at bay. The same barriers that push seniors into food banks also pull them away from neighbours, faith communities and civic life.
Canada is moving toward a super-aged reality, with more than 8.1 million people already 65 or older. For Ontario, that should change how food banks, municipalities and provincial policy think about senior dignity. A food program is not just about calories. It is about whether an 82 year old widow is greeted by name, whether she can sit for coffee instead of rushing through a line, whether transportation and home supports let her stay rooted in the community she helped build.
In practice, that means treating food banks as community hubs for older adults. Local riding associations, unions, faith groups and senior clubs can partner to offer warm spaces where meals, mental health check ins and peer connection happen side by side. Intake questions can be designed to connect people to housing help, home care information and social programs, not to shame them for needing a bag of groceries.
Here is the evidence base behind this argument.
Research-based facts: about 20 per cent of Canadians 50 and older live at a material deprivation level; 18 per cent cannot afford a 500 dollar expense; 11 per cent report being unable to afford dental care; 43 per cent are at risk of social isolation and 57 per cent feel lonely; senior food bank use has increased 35 per cent since 2023; more than 8.1 million people in Canada are 65 or older.
Practice-based observations: seniors often trade nutrition to keep up with rent and utilities; transportation costs frequently decide whether an older person can attend social or community programs; food banks that provide seating, conversation and information tables tend to see regulars staying longer and reporting greater emotional relief.
Interpretive recommendations: food insecurity and loneliness among seniors should be treated as linked public health issues; food banks can be repositioned as dignity-first community hubs for aging; provincial policy and local organizing in Ontario should prioritise transportation, social connection and respectful intake as core parts of senior food programs.
For Ontario’s seniors, the fight for dignity in aging runs straight through food insecurity, social isolation and mental health. When one in 5 older adults is living at a poverty-level standard of living, there is no neutral ground. Governments, communities and political movements that claim to stand for public service have a choice: treat food banks as a permanent backstop for the poor, or turn them into bridges to a future where elders are fed, connected and fully respected.
If you haven't yet signed up for our OLSC bi-weekly newsletter, SUBSCRIBE or better yet, help other seniors as a VOLUNTEER.
This article was created using research from the cited references below, a human editor and an AI-assisted workflow.